

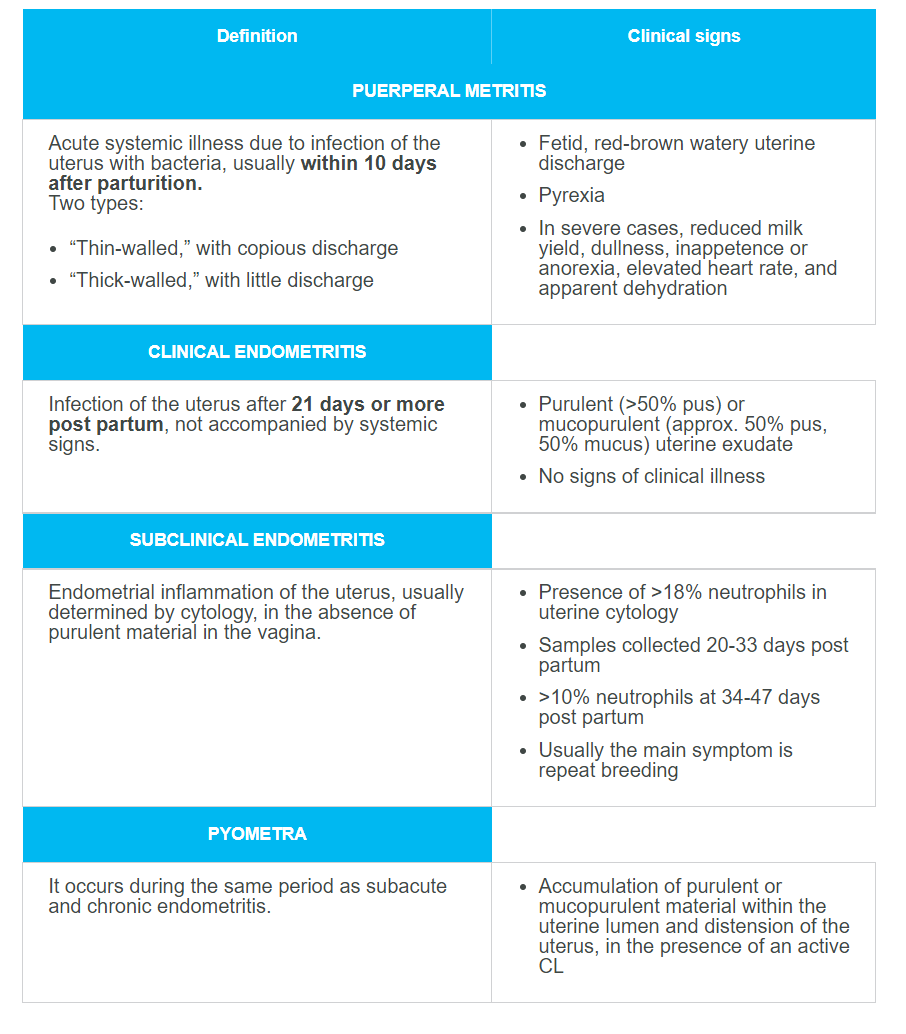
Endometritis
Infection of the uterus without any detectable symptom.
Abnormal births:
- Assisted calvings
- Induced calvings
- Dead calves/stillbirths
- Twins
- Retained fetal membranes
Metabolic disorders:
- Milk fever
- Ketosis
- Fatty liver syndrome
- Displaced abomasum
Postpartum Uterine Disease in Cattle1
In most cows uterine involution is a septic process. Bacteria are found to invade the uterus during the first two weeks post partum. Whether the uterus overcomes this infection depends on the number and virulence of the bacteria present, condition of the uterus, and the quality of natural defense mechanisms.
In the course of a normal postpartum, a cow cures a uterine infection by rapid involution of the uterus and cervix, discharge of uterine contents and mobilization of natural host defense, including mucus, antibodies and phagocytic cells.
The uteri of cows with periparturient problems are larger and require three to five days longer for involution than the uteri of normal cows. These cows will have a reduced ability to control uterine infections.
If parturition is prolonged or assistance is needed2, the chances for bacterial infection increase.
- Excessive stretching of the uterus (e.g., hydrops allantois or twins)
- Traumatic injury of genitals during dystocia or obstetric manipulations
- Metabolic disorders
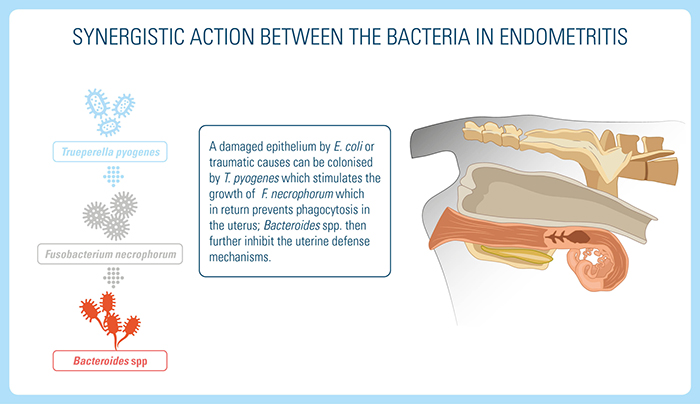
The concomitant high prevalence of T. pyogenes and Gram-negative anaerobic bacteria seems to be related to the severity of endometritis and suggests a synergistic action between the bacteria.
- Clinical history
- Visual inspection (discharge)
- Rectal examination
- Vaginoscopy: More accurate but less practical method than rectal palpation or vaginal inspection for determining the presence of subacute and chronic endometritis
- Use of Metricheck® device
Intra-uterine treatment with antibiotics can be effective if:
- The antibiotic has the right spectrum for the main pathogens
- The concentration at the site of inflammation is high enough
- The antibiotic does not inhibit the natural defense of the uterus
Administrating prostaglandin F2α or its analogues at normal luteolytic doses is the treatment of choice for pyometra in cattle. No intrauterine treatment is recommended in conjunction with the prostaglandin3.
- Sheldon, I.M., Lewis, G.S., LeBlanc, S., Gilbert, R.O. 2006. Defining postpartum uterine disease in cattle. Theriogenology. 65(8):1516-30.
- Dohmen, M.J.W., Lohuis, J.A.C.M., Huszenicaza, G.Y., Nagy, P., Gacs, M. 1995. The relationship between bacteriological and clinical findings in cows with sub acute / chronic endometritis. Theriogenology, 43; 1379-1388.
- Gilbert, R.O. https://www.msdvetmanual.com/reproductive-system/metritis-in-large-animals/pyometra-in-large-animals. MSD Veterinary Manual.

